Artigo publicado na BMJ Case Reports 2012; doi:10.1136/bcr-2012-006430
Atypical ‘benign behaviour’ of eyelid sebaceous carcinoma
Samuel Alves, Filipe Silva, Mara Ferreira, João Cabral
Department of Ophthalmology, Hospital Prof. Dr. Fernando Fonseca, Lisboa, Portugal
Summary
Eyelid sebaceous carcinoma is a rare tumour with slow growth and it is one of the most aggressive malignancies of the eyelid. Death rate can reach 6%. The diagnosis is often delayed because it is confused with other periocular lesions. The authors describe a case with atypical presentation, regarding rapid growth rate and exophytic aspect. Female, 78 years, presenting lower eyelid tumour with 4 months of evolution. Ophthalmological examination showed a tarsal exophytic tumour (22 mm), non-adherent to bulbar conjunctiva. She was medicated topically for 3 months, with the diagnosis of chalazio. Total excision was performed for histological diagnosis. After diagnosis of sebaceous carcinoma with specific immunohistochemical markers, and without free tumour surgical limits, a second surgery was performed with a pentagon entire thickness excision. Being a rare tumour but with a considerable morbidity and mortality; early diagnosis and treatment is essential for a good prognosis and preservation of visual function.
Background
Rare case of eyelid sebaceous carcinoma (SC) with a rare clinic presentation.
Case presentation
A 78-year-old female patient, complaining of lower eyelid tumour lesion with 4 months evolution. Three months before, it was diagnosed as a chalazio, been treated topically with corticosteroids and antibiotic ointment. Despite the therapy, eyelid mass continued to grow. One month ago she decided to visit our hospital.
Ophthalmological examination showed a solid tumour in the inferior tarsal conjunctiva, exophytic and pedunculated, non-adherent to bulbar conjunctiva. The macroscopic tumour appearance was multilobulated yellowish heterogeneous mass with a size of about 20 mm (Fig. 1). Remaining examination without other findings, including lack of preauricular, parotid, submandibular and cervical adenopathy.
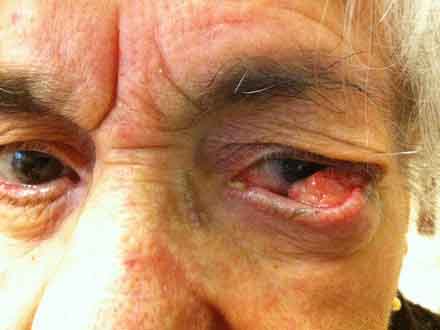
Figure 1: Eyelid tumor at presentation.
After gentle manipulation of the lower eyelid the tumour mass went out of the orbital cavity, anterior to the lid fissure (Fig. 2).

Figure 2: Tumor extrusion after gentle manipulation of lower eyelid.
The reduction to the starting position was impossible, so we decided to move to total excision of the mass in the same day and posterior histological diagnosis.
Investigations and treatment
The surgical specimen had dimensions of 2.2 ×1.5 ×1 cm (Fig. 3).
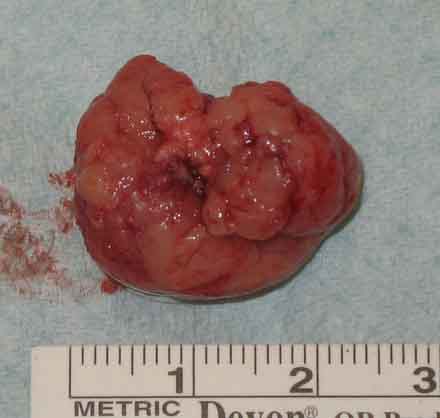
Figure 3: Tumor after extraction.
Histopathological examination concluded: ‘tumour compatible with sebaceous cell carcinoma (Cam 5.2, CK7, EMA-epithelial membrane antigen, Ber-ep4 positive for immunohistochemistry) with Ki67 and p53 proliferative index in more than 70% cells’ (Fig. 4-6).
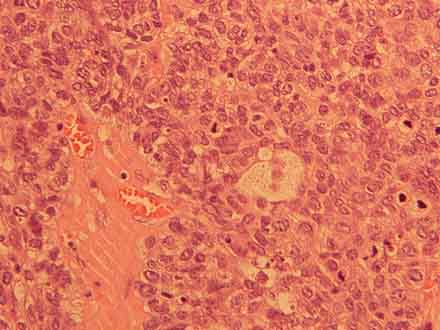
Figure 4: Proliferation of atypical cells, some with pale vacuolated cytoplasm (HE 200x).
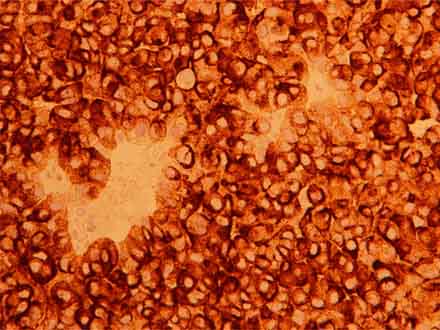
Figure 5: Positive immunostaining with epithelial membrane antigen (EMA 200x).
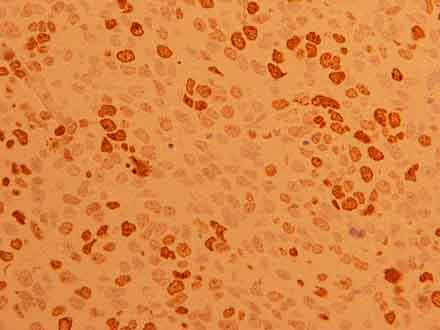
Figure 6: Immunostaining of numerous nuclei, indicating a high proliferative index (Ki67 200x).
After histological diagnosis of SC without safe surgical limits, it was performed a second surgery with pentagonal excision of the entire eyelid thickness and direct closure. The final functional and aesthetic result was very good. The histological results showed margins free of carcinoma.
Outcome and follow-up
As a rare tumour, SC has a considerable mortality (up to 6%)1 and a high rate of local recurrence and risk of metastasis (30%).2 On the contrary, in this case, the diffuse and invasive growth pattern was not observed, which resulted in a better surgical outcome and better overall prognosis.
Despite the exuberance of the tumour, the only poor prognosis factors were diameter >10 mm and p53 overexpression.2
The patient is monitored in ophthalmology every 3 months with a follow-up of 6 months at this point. It was also referred to oncology for systemic metastases screening.
Discussion
Despite the atypical pedunculated tumour with rapid growth, the diagnosis of SC was confirmed histologically.
The SC, which often develops in the periocular (75%) area is a rare tumour. The remaining 25% SC are normally located in the head and neck, including parotid gland. SC corresponds to 0.2-0.8% of all eyelid tumours, and about 1-5.5% of the eyelid malignancies. In China and India the incidence of SC is higher than in Europe and USA (which may reach around 50% of eyelid malignancies, contributing also the low incidence of BCC).
It is a slow-growing tumour that usually affects older people with a predominance in women. It develops from the sebaceous glands of meibomian, of Zeis, caruncle or hair follicles. Most often located in the upper eyelid due to the greater number of meibomian glands.
Clinically, it can have different presentations1-3, including eyelid solitary nodule, pseudo-inflammatory pattern, diffuse, pedunculated lesion, caruncle, eyebrow or lacrimal gland tumour and rarely an extensive orbital invasive pattern.
The diagnosis is often delayed once it simulates several other benign conditions such as blepharoconjunctivitis, chronic relapsing chalazio. Moreover, SC can simulate other tumours such as basal cell carcinoma, squamous cell carcinoma, melanoma, Merckel neuro-endocrine carcinoma or lymphoma.
The final diagnosis is made histologically2,3 by the presence of typical cytoplasmic lipid vacuoles and glandular neoplastic cells with prominent nucleoli. SC has a characteristic immunohistochemical profile, similar to that of the breast tumours, and is useful for diagnosis markers such as HMFG1 (human milk fat globule-1) or EMA.
About 30% of SC metastasise.2 The typical way of SC metastasis is the lymphatic vessels to regional lymph nodes of head and neck. The upper eyelid SC metastasise to the parotid and ear region, while the lower eyelid SC invade submandibular or cervical lymph nodes. The haematogenous way is rare. The death rate for metastatic disease can reach 6%.1
Among the poor prognosis factors3 is included the diffuse intraepithelial invasion (‘Pagetoid spread’), poor histological differentiation, infiltrative, multifocal origin, tumour diameter exceeding 10 mm, vascular or lymphatic invasion, orbital invasion, simultaneous involvement of upper and lower eyelid and symptomatic tumour more than 6 months. It is believed in the future that overexpression of oncosupressor p53 gene will be a marker for more aggressive disease.2
